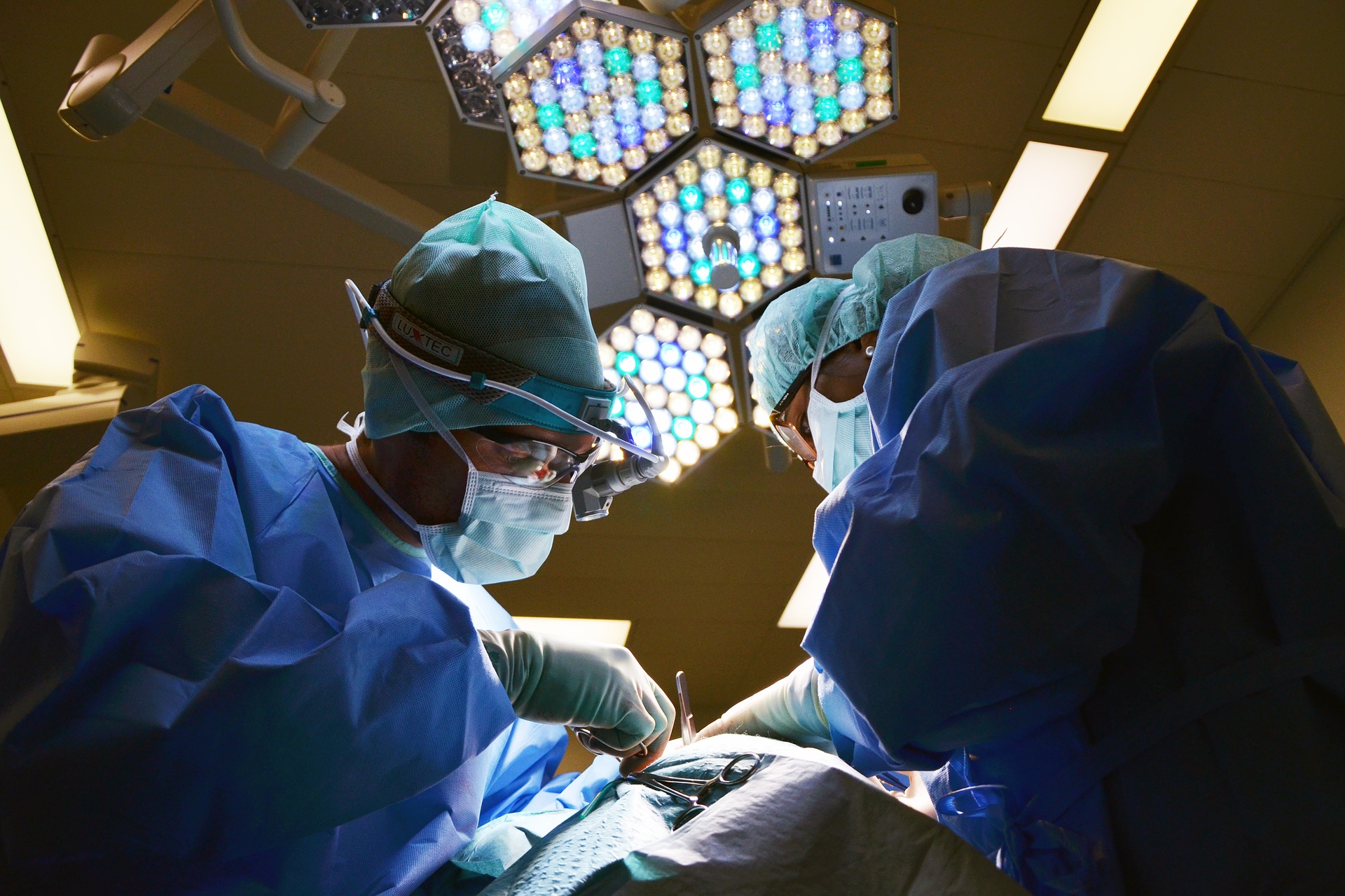
Boo! Being a Physician Can Be Downright Scary
This post may contain links from our sponsors. We provide you with accurate, reliable information. Learn more about how we make money and select our advertising partners.
What better way to kick off the week before Halloween than to share scary OR stories. I was never that enthusiastic about this holiday until I had children. Now it's something I look forward to every year.
As you may know, as an anesthesiologist, things are great… until they're not. See what I mean below, enjoy!
Today's Classic is republished from Physician on Fire. You can see the original here.
You won’t find me at any haunted houses this Halloween. I don’t need any costumed creeps jumping out at me when I least (or most) expect it. I’ve never been a huge fan of strobe lights, fog machines, bad makeup, or canned Vincent Price laughter.
My day job is scary enough.
Some like to say that anesthesia is 99% boredom and 1% terror. They’re half right. The 99% is rarely boring. The “routine” part of my workday is usually quite busy, sometimes fun, and never boring. The terror part? I used to deny it, but as I reflect on my career, I am willing to admit that rare moments do indeed qualify as terrifying.
Exhibit A: The Blood Sugar is 11
On a ten point scale, 11 is off the charts in a good way. On a hypoglycemia level, 11 is absolutely frightful. Earlier this year, I was finishing up the placement of a labor epidural when I was called to come to the nursery. Conveniently, I was just down the hall. There was a newborn, with her tiny fingers, toes, and veins in need of an IV for an urgently needed dextrose infusion.
The nurses had made a couple of attempts, but to no avail.
There was one visible vein remaining — on her left foot — and time was of the essence. I poked once with a 24-gauge IV. Nothing. Another attempt a few millimeters proximal, and I struck crimson gold. Sugar was given, the baby perked up, and a crisis was averted.
Earlier in my career, a patient undergoing a kidney transplant developed a markedly elevated potassium, as evidenced by telltale EKG changes. I treated her with the usual remedies, including dextrose and insulin. The potassium dropped, but there were new EKG changes (that telltale heart again).
A blood draw confirmed what I suspected — profound hypoglycemia — it wasn’t 11, but it wasn’t much higher. Dextrose provided a quick fix, but I’ll tell you I was quite relieved when she woke up postoperatively and could carry on a normal conversation. The heart doesn’t like to be without fuel; the brain doesn’t either.

pumpkin carving templates make me look skilled
Exhibit B: Beep bleep bloop
Every patient under our care is equipped with continuous pulse oximetry, a technology typically employing a finger clip that approximates the patient’s level of oxygen in the bloodstream. The “beep… beep… beep” you hear on Grey’s Anatomy? That’s the pulse ox. At a normal range of 97% to 100%, it’s a high-pitched beep. As it drops, the pitch lowers. Our brains are attuned to notice even a slight alteration in pitch.
Sometimes, the drop in pitch isn’t so slight. Sometimes, the subwoofer kicks in. This is not good. Not good at all. A patient’s oxygen can drop rapidly for a few dozen different reasons, and when it does, correcting the problem is the only priority. When the O2 sats hit the floor, you’ve got seconds before the heart can start to malfunction. In minutes, there can be brain damage.
Fortunately, we have all sorts of equipment to aid us in a rescue situation. There are facemasks, breathing tubes and similar devices, and a wide variety of tools to assist us in placing those tubes in the right place. When they’re needed, they’re needed now.
When have I needed them? When called to the room of a trainee who inadvertently over-sedated a patient undergoing a minor procedure and failed to timely recognize it. When a super obese (yes that’s an actual medical term for a BMI > 50) patient proves extraordinarily difficult to intubate. When the EM or ICU physician has failed to find the larynx using every tool at his disposal. When a newborn baby has poor respiratory effort and isn’t “pinking up.” When a toddler arrives essentially DOA after a horrific car accident.
Those are just a few of the dozens of precarious situations I’ve faced over the last decade. Thankfully, I’ve always been able to do what needed to be done, and it’s not just because I’ve been well trained. I’ve relied on the assistance of many a colleague. That fact that we’ve achieved success in the past doesn’t make the next situation any easier, and the images of those patients never leave you. To my dying day, I will never forget that doll-eyed toddler.

Exhibit C: Blood and Guts
I’ve never been bothered by the sight of blood and guts. They’re the bread and butter of what we see and do in the operating room. Mangled fingers and bone exposed from injury do make me cringe a bit, but the splayed open belly is just another day at the office. What I don’t like is when those patients try their darndest to die on you.
I work in a community hospital. Major trauma patients are flown out to better-equipped trauma centers. I have great respect for the physicians who care for near-death patients on a daily basis. Frankly, the stress would do me in. There’s a reason I work at a community hospital.
That being said, we do care for crashing patients on occasion.
The emergency belly cases tend to be one of two varieties. There is the septic ICU patient whose blood pressure has been maintained on maximum levels of several pressors, who has a belly full of dead bowel spilling all sorts of evil humors into the blood stream that tend to be incompatible with life. I wrote in detail about one of these cases in We Were Promised Death Panels.
The other is a bleeder. These patients are scarier, because unlike the dead bowel patient, this patient was probably reasonably healthy before she started bleeding. She could be bleeding from an internal process, such as a ruptured ectopic pregnancy. It might be from a spleen or liver lacerated from trauma. The cause could be iatrogenic, that is, caused by a surgical or medical mishap.
Regardless of the cause, this patient will have no blood pressure or pulse without generous and continuous intravenous fluids and blood products. When the pace of bleeding exceeds the pace at which you can replace the losses, you’ve got precious little time to obtain better access. This is when we literally go for the jugular, inserting large bore catheters into the jugular vein to allow for a steady stream of fluids and blood that can be infused at a liter a minute or more.
Once again, the teamwork makes a good outcome possible, but the continual manual labor, consuming thought process, and constant threat of a negative outcome makes these cases physically and mentally exhausting.
Welcome to My Scary Life
I could write another 10,000 words on just how frightful a physician’s workday can be, but I think I’ve gotten the point across. On one hand, I take pride in the fact that I face these scary moments on a semi-regular basis, and can handle them with at least a semblance of confidence and calm. It’s a learned behavior. To be honest, though, every scary moment comes with an adrenaline rush that’s impossible to dismiss. Some physicians live for it; I live to avoid it.
There will be at least a few more moments of terror in the one more year before I set aside the laryngoscope. I can accept that, but if I could finish out my career without another scary moment, I would enter into early retirement a happy man.
Disclaimer: The topic presented in this article is provided as general information and for educational purposes. It is not a substitute for professional advice. Accordingly, before taking action, consult with your team of professionals.



