
Why I Don’t Plan on Quitting Medicine Anytime Soon
This post may contain links from our sponsors. We provide you with accurate, reliable information. Learn more about how we make money and select our advertising partners.
I feel fortunate to have been turned on to the idea of multiple streams of passive income early on in my career. It took a combination of struggling to find security at work, reading a few good books, and speaking to some doctors who had escaped the “rat race” to put me on this journey to financial freedom.
I now know the impact it can have on the enjoyment and longevity of one's medical career, and that's why I'm so passionate about sharing this concept with others.
However, when I start talking to people about my various business ventures, streams of income, and the financial freedom they can bring, one question always seems to pop up, “When are you going to quit being a doctor?” To which my response is always the same, “Never… I hope.”
Why Leave Medicine
We all know that, in many ways, being a physician is tougher today than ever before. With so many bureaucratic tasks like charting and paperwork required of us, increased hours of work with less pay, a decreasing lack of respect at work, lack of control and autonomy, increased regulations to abide by, etc., it’s no wonder that physician burnout is on the rise.
In fact, in a recent Medscape survey, 44% of physicians who responded (>15,000 physicians) admitted to feeling burned out. They defined burnout as: “long-term, unresolvable job stress that leads to exhaustion and feeling overwhelmed, cynical, detached from the job, and lacking a sense of personal accomplishment.” I'm sure that some of you can relate to this.
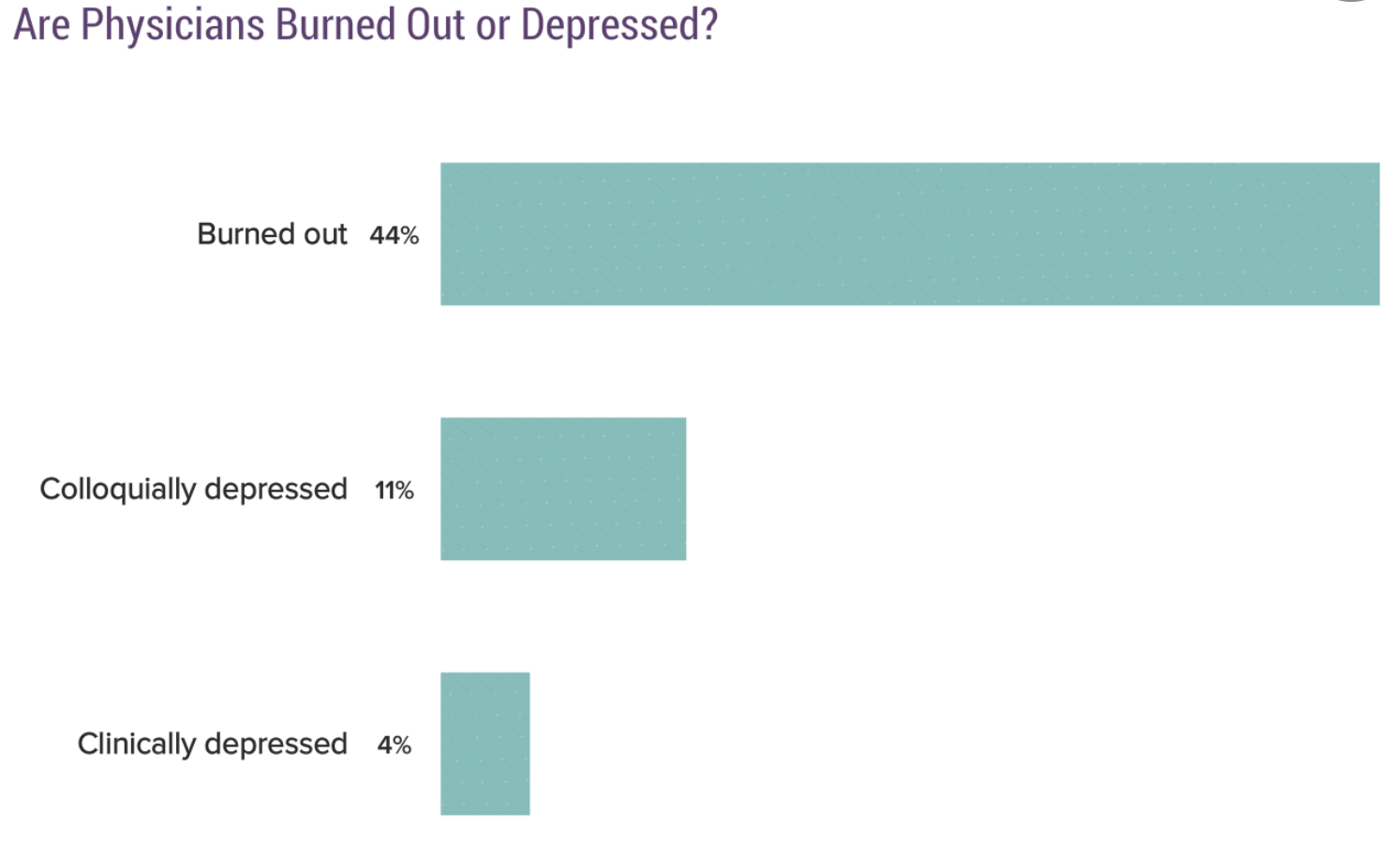
As a result, many physicians are leaving the workplace, and there are so many more who might leave if not for financial obligations. Burnout added on top of large student loan debt, mortgages, car payments, and kids' education costs… it all leads to the feeling of being trapped.
That makes me wonder – if finances truly weren’t an issue (for example, if they won the lottery), just how many physicians would continue to practice medicine?
My hope is that many of them would continue being physicians. Perhaps having that financial freedom could change the way they practice into something a lot more sustainable – work fewer hours, and/or spend more time with individual patients. This might rekindle some sort of lost passion for their field.
Some Stay, Some Leave
Some of my friends, like the White Coat Investor, have reached that point of financial independence but continue to work because they want to, albeit a reduced amount. Others, like Physician on Fire, expect to make a complete exit from medicine very soon.
Whatever anyone chooses though, I believe it’s not my place to judge. Everyone must figure out what works for them. After all, your job is important, but I believe it’s not the most important thing in life. (If you want to talk philosophical about the meaning of life, let's talk about it in our group, Passive Income Docs.)
Perhaps if you're in one of the specialties more prone to burnout, you're more likely to leave if given the choice.
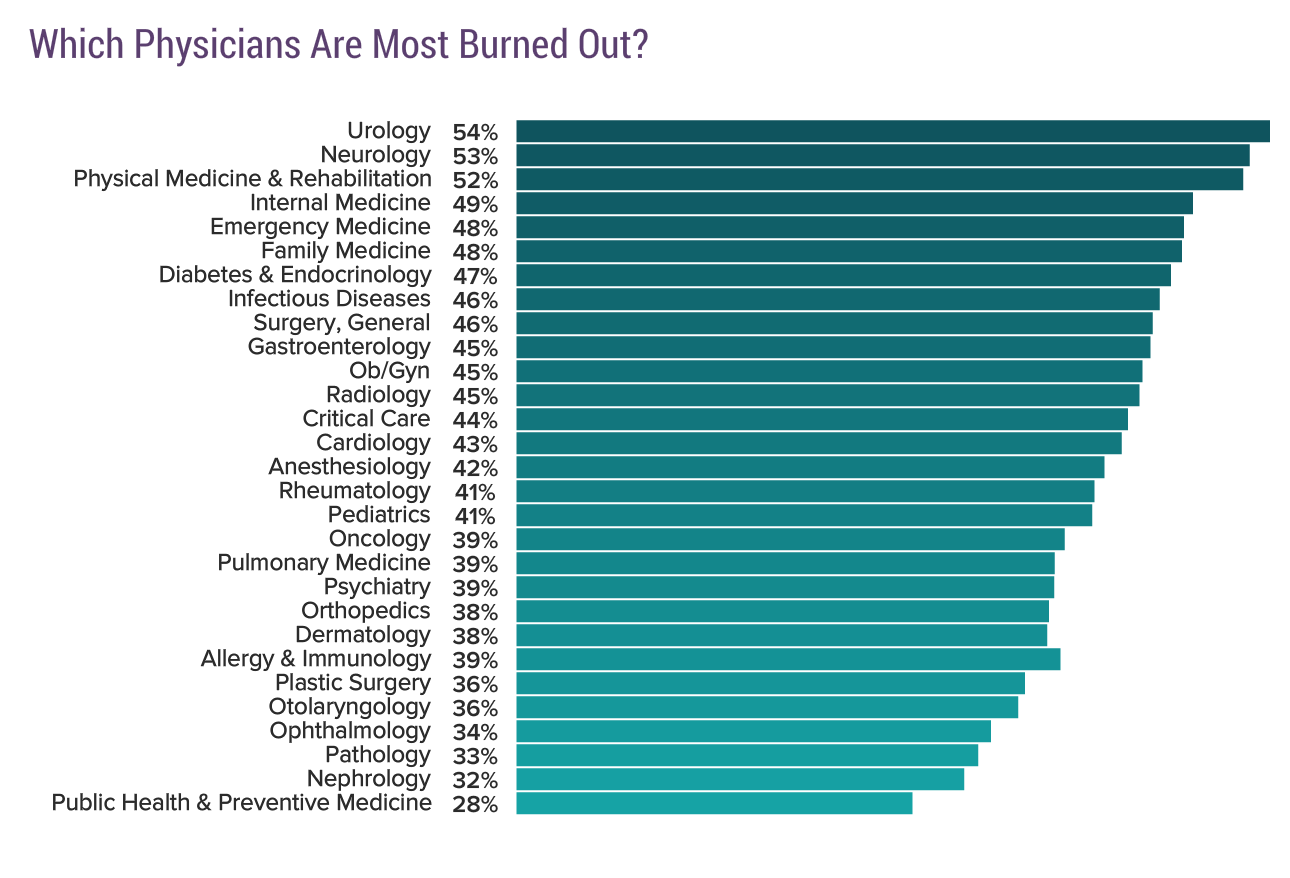
However, even though I'm in a field that experiences a relatively higher chance of feeling burned out (Anesthesiology), I feel like I want to keep going. In spite of having that choice to leave medicine, I hope to never quit my job.
Here are some of the reasons why:
Working Still Makes Me Feel Good and Gives Me a Sense of Purpose
I actually enjoy what I do. I’m a fellowship-trained obstetric anesthesiologist. Yes, there aren't too many of us around, but it's a great field. Just ask our society!
I chose this particular field because, at the end of the day, nothing could match that feeling of satisfaction I received at the end of an OB shift. I get to help people through a very stressful time and in some way, I feel it's what I'm meant to do.
Plus, if there’s one place in a hospital where people actually want to be, it’s Labor & Delivery. It's a happy place and although it can be quite busy, the cupcakes, balloons, and happy hugs still rub off positively on me.
Lastly, call me a softie, but it still gets me when I see parents with their newborn babies. I loved it before having kids, but now having had my own, it's that much more meaningful.
It’s Challenging and Intellectually Stimulating
I enjoy the challenge that my job provides. I perform very technical procedures like epidurals and spinals, and I like to think I do it decently well. Then there’s the challenge of managing the patient through some difficult moments.
Ultimately, people need to be constantly challenged and stimulated to grow. I’ve heard that once people stop being challenged, they wither away. This is why retirement becomes such a struggle for a lot of people.
Of course, I do get that stimulation from certain other ventures, like this blog and the other businesses, but being able to work that while also helping people is immensely satisfying.
I Enjoy Teaching
I work with residents and fellows on a daily basis and there’s something special about the feeling of contributing to someone’s education and training. When I hear of one of our former residents or fellows doing well out there in the world, there’s a sense of pride that comes with knowing that I helped to train that person.
I Like the People I Work With
My colleagues are good people who work hard. I’ve made good friendships while working at my hospital, and though we don’t always hang out outside of work, I still feel comfortable calling them if I needed anything. Of course, I'd do the same for them.
I also get to interact with patients, other physicians, nurses, and staff on a daily basis, and it’s a very collegial atmosphere.
I Enjoy the Income
My work provides a steady income for the most part. The good part about getting paid for your time is that you know how much you will receive at the end of a shift. The bad part is that since most medical income is tied to time, you'd always be captive to your work if you didn't have any other income streams.
Again, thankfully I do have some other sources of income, but it's not always consistent at this point. The medical income is a nice buffer in case things don’t go so well with the businesses or my investments. That extra income is usually thrown into more investments, but it also allows me to take care of my family members that much easier. Oh, and I do enjoy traveling quite a bit and my day job makes it easier on the finances to do so.
What Could Drive Me to Quit
I know I painted quite a rosy picture of my current day job, but in all honesty, it's not always smooth. But I'm definitely a glass-half-full type of guy. I recognize no situation is perfect, but I'm very fortunate to have what I have. That isn't to say things couldn't change as I've seen it has for some of my friends. In fact, there are things that could drive me to quit prematurely. Some of those things are:
Loss of Flexibility
Well, the major thing that could make me quit is if I lost flexibility. If I didn't have the time in my week to pursue some of my other ventures or if I was forced to work 60-70 hours a week, then the decision to stay in medicine would be quite a bit more difficult.
Liability
I might also hang up my stethoscope if the threat of lawsuits was constant or real enough to make me think I could potentially lose everything.
Physical Limitations
My job is very technical so if I were physically unable to perform the tasks well I wouldn't be doing a service to anyone. A career-ending accident could happen, but that's also why I have good disability insurance.
Gradual Retirement
So even though I’ve reached financial independence from medicine, instead of retiring immediately, I’ve decided to gradually retire. That means that as my income increases from other ventures, I’ve decreased my time at work.
I’ve decided to take this step immediately because it's clear that work hours and burnout are directly correlated. If I decided to wait until I reached a certain amount of income or level of comfort before reducing my time, I feel I'm way more likely to hit that burnout wall. So I'm pushing myself to work less.
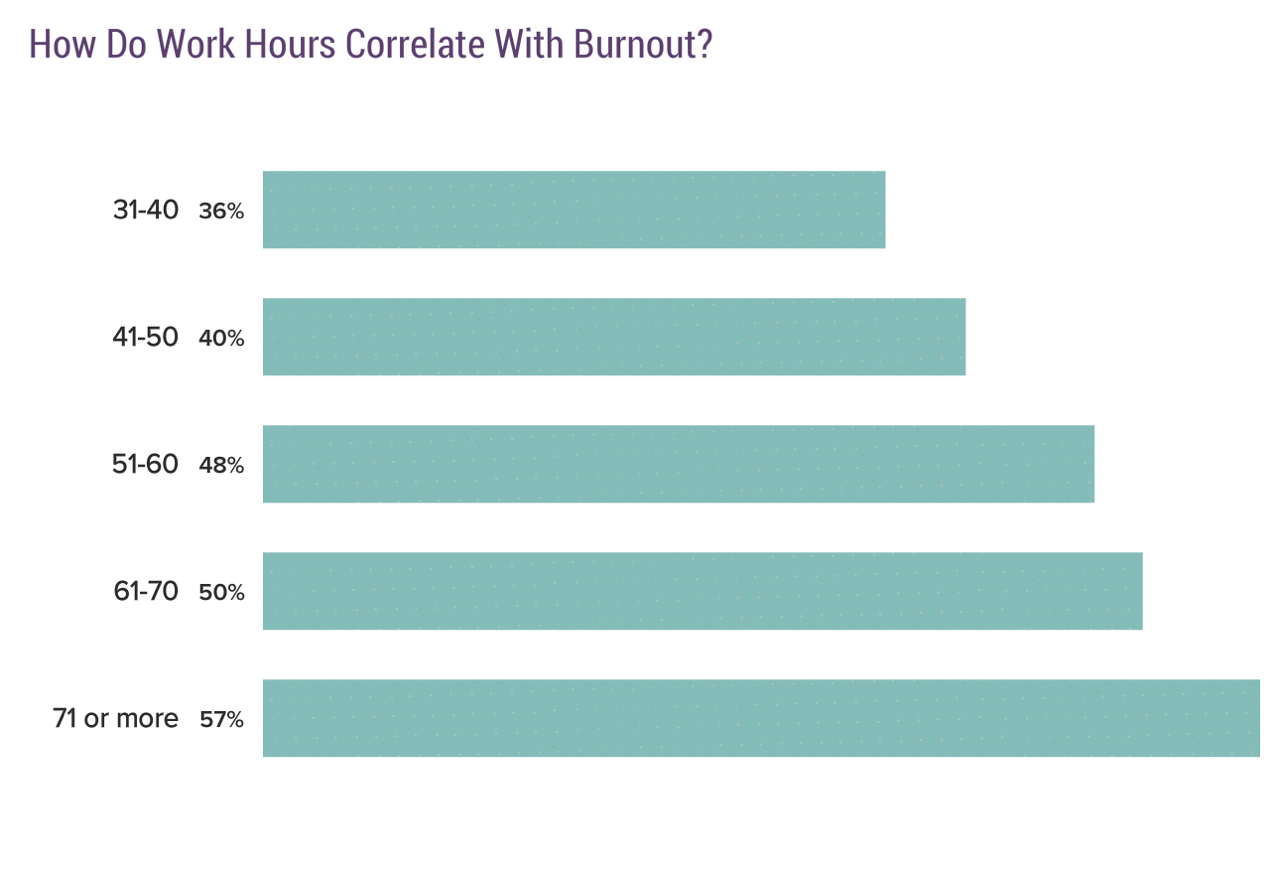
I’m dropping hours as I go and opting to spend more time with family and on other ventures.
I'm not saying this is the only solution to burnout. I don't pretend to have all the answers because the causes and solutions to burnout in medicine are multifactorial. I've just found what works for me.
But one thing’s for certain, I won’t be completely quitting medicine anytime soon.
If you reached financial freedom, would you quit practicing completely? Or would you gradually retire?

Disclaimer: The topic presented in this article is provided as general information and for educational purposes. It is not a substitute for professional advice. Accordingly, before taking action, consult with your team of professionals.



